Hypocalcemia / Diabetic Ketoacidosis . Hypercalcemia also spelled Hypercalcaemia is a high calcium (Ca2+) level in the blood serum. Those with a mild increase that has developed slowly typically have no symptoms. In those with greater levels or rapid onset, symptoms may include abdominal pain, bone pain, confusion, depression, weakness, kidney stones, or an abnormal heart rhythm including cardiac arrest.
Diabetic ketoacidosis (DKA) is a potentially life-threatening complication of diabetes mellitus. Signs and symptoms may include vomiting, abdominal pain, deep gasping breathing, increased urination, weakness, confusion, and occasionally loss of consciousness. A person’s breath may develop a specific smell. Onset of symptoms is usually rapid. In some cases people may not realize they previously had diabetes.
DKA happens most often in those with type 1 diabetes, but can also occur in those with other types of diabetes under certain circumstances. Triggers may include infection, not taking insulin correctly, stroke, and certain medications such as steroids.[1] DKA results from a shortage of insulin; in response the body switches to burning fatty acids which produces acidic ketone bodies. DKA is typically diagnosed when testing finds high blood sugar, low blood pH, and ketoacids in either the blood or urine.
Most cases are due to primary hyperparathyroidism or cancer. Other causes include sarcoidosis, tuberculosis, Paget disease, multiple endocrine neoplasia (MEN), vitamin D toxicity, familial hypocalciuric hypercalcaemia, and certain medications such as lithium and hydrochlorothiazide. Diagnosis should generally include either a corrected calcium or ionized calcium level and be confirmed after a week. Specific changes, such as a shortened QT interval, may be seen on an electrocardiogram
Hypocalcemia also spelled hypocalcaemia is low calcium levels in the blood serum. The normal range is 2.1–2.6 mmol/l (8.8–10.7 mg/dl, 4.3–5.2 mEq/l) with levels less than 2.1 mmol/l defined as hypocalcemia. Mildly low levels that develop slowly often have no symptoms. Otherwise symptoms may include numbness, muscle spasms, seizures, confusion, or cardiac arrest.
Common causes include hypoparathyroidism and vitamin D deficiency. Others causes include kidney failure, pancreatitis, calcium channel blocker overdose, rhabdomyolysis, tumor lysis syndrome, and medications such as bisphosphonates. Diagnosis should generally be confirmed with a corrected calcium or ionized calcium level. Specific changes may be seen on an electrocardiogram (ECG)
Calcium Homeostasis
Fraction
- 15% bound to anions (phosphate, lactate, citrate)
- 40% bound to albumin
- 45% free (regulated by PTH, Vit-D)
Conditions causing changes in total calcium (without affecting ionized calcium)
- Low albumin causes hypocalcemia. Corrected = measured + [0.8 x (4-albumin)]
- Elevated albumin causes hypercalcemia
- Multiple myeloma causes hypercalcemia
Conditions causing changes in ionized calcium (without affecting total calcium)
- Alkalemia causes increased ionized calcium binding to albumin and decreases ionized calcium levels
- Hyperphosphatemia causes increased ionized calcium binding to phosphate and decreases ionized calcium levels
- Hyperparathyroidism causes decreased ionized calcium binding to albumin and increases ionized calcium levels
Causes of Hypocalcemia
- Eating disorders
- Prolonged vomiting (e.g. with a viral illness)
- Exposure to mercury, including infantile acrodynia
- Excessive dietary magnesium, as with supplementation.
- Excessive dietary zinc, as with supplementation (causes rapid hypocalcemia).
- Prolonged use of medications/laxatives containing magnesium
- Chelation therapy for metal exposure, particularly EDTA
- Osteoporosis treatment or preventive agents, such as bisphosphonates and denosumab.
- Agents for the treatment of hypercalcemia, such as Calcitonin.
- Chronic kidney failure
Absent active vitamin D
- Decreased dietary intake
- Decreased sun exposure
Defective Vitamin D metabolism
- Anticonvulsant therapy
- Vitamin-D dependent rickets, type I
Ineffective active vitamin D
- Intestinal malabsorption
- Vitamin-D dependent rickets, type II
- Pseudohypoparathyroidism
- Severe acute hyperphosphataemia
- Tumour lysis syndrome
Acute kidney failure
- Rhabdomyolysis (initial stage)
- Exposure to hydrofluoric acid which can be fatal if 2.5% of skin is exposed
- As a complication of pancreatitis
- Alkalosis, often caused by hyperventilation
Symptoms
| ACUTE | CHRONIC |
|---|---|
Neuromuscular
Cardiac
|
CNS
Ophthalmologic
|
Additional symptoms
- Petechiae which appear as on-off spots, then later become confluent, and appear as purpura(larger bruised areas, usually in dependent regions of the body).
- Oral, perioral and acral paresthesias, tingling or ‘pins and needles’ sensation in and around the mouth and lips, and in the extremities of the hands and feet. This is often the earliest symptom of hypocalcaemia.
- Carpopedal and generalized tetany (unrelieved and strong contractions of the hands, and in the large muscles of the rest of the body) are seen.
Latent tetany
- Trousseau sign of latent tetany (eliciting carpal spasm by inflating the blood pressure cuff and maintaining the cuff pressure above systolic)
- Chvostek’s sign (tapping of the inferior portion of the cheekbone will produce facial spasms)
- Tendon reflexes are hyperactive
Life-threatening complications
- Laryngospasm
- Cardiac arrhythmias
Effects on cardiac output
- Negative chronotropic effect, or a decrease in heart rate.
- Negative inotropic effect, or a decrease in contractility
ECG changes include the following
- Intermittent QT prolongation, or intermittent prolongation of the QTc (corrected QT interval) on the EKG (electrocardiogram) is noted. The implications of intermittent QTc prolongation predisposes to life-threatening cardiac electrical instability (and this is therefore a more critical condition than constant QTc prolongation). This type of electrical instability puts the patient at high risk of torsades de pointes, a specific type of ventricular tachycardia which appears on an EKG (or ECG) as something which looks a bit like a sine wave with a regularly increasing and decreasing amplitude. (Torsades de pointes can cause death, unless the patient can be medically or electrically cardioverted and returned to a normal cardiac rhythm.)
Management
Severe (symptomatic, QT prolongation)
- Calcium gluconate 1-2g IV in 50mL of D5W over 10-20min followed by slow infusion of additional 2g over 2 hours.
Asymptomatic
- Calcium gluconate 1g PO q6hCalcitriol 0.2mcg PO BID
Diabetic Ketoacidosis
HPI
30 year-old female with a history of autoimmune polyglandular syndrome (adrenal, thyroid and endocrine pancreatic insufficiency), polysubstance use, brought to the emergency department by ambulance with reported chief complaint of fever. On presentation, the patient reported fever for one day, associated with cough. She was lethargic and confused, answering yes/no questions but unable to provide detailed history. She states that she has been taking her home medications as prescribed, which include hydrocortisone, fludrocortisone, synthroid and insulin. No collateral information was immediately available.
Additional history was obtained from chart review upon discharge. The patient was hospitalized two weeks prior with pneumonia and discharged after two days. For 2-3 days prior to presentation, she reported the following symptoms to family members: nausea/vomiting, cough, decreased oral intake, fevers, and palpitations – she did not take her home medications during this time.
Physical Exam
| VS: | T | 38.6 | HR | 112 | RR | 18 | BP | 149/82 | O2 | 90% RA |
| Gen: | Alert, fatigued, slow responses. | |||||||||
| HEENT: | No meningeal irritation, dry mucous membranes. | |||||||||
| Pulmonary: | Tachypnea, inspiratory wheezing and faint crackles at left and right inferior lung fields, appreciated anteriorly as well. | |||||||||
| Neuro: | Alert, oriented to self, situation, not month/year. PERRL, EOMI, facial muscles symmetric, tongue protrudes midline without fasciculation. Peripheral sensation grossly intact to light touch and moves all extremities on command. | |||||||||
Labs
- VBG: alkalemia, primary respiratory
- CBC: no leukocytosis, normal differential, normocytic anemia
- BMP: 131, 2.5 , 94, 28, 11, 1.6, 115
- Mg: 1.3
- Lactate: 1.0
- TSH: 17 , T4: 1.03
- Troponin: 0.129
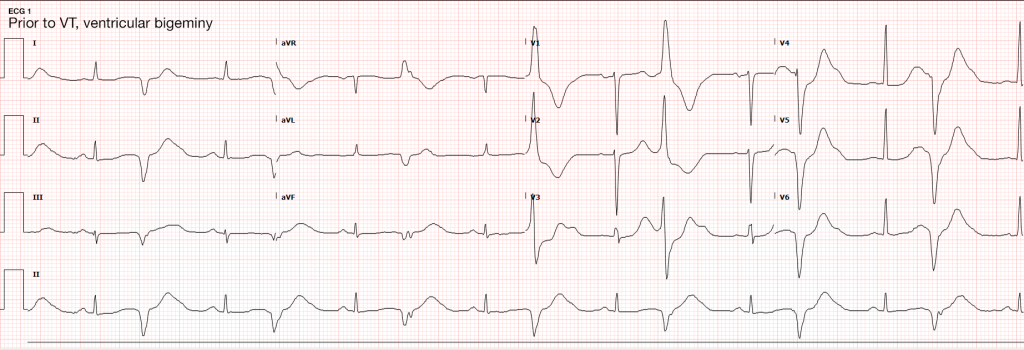
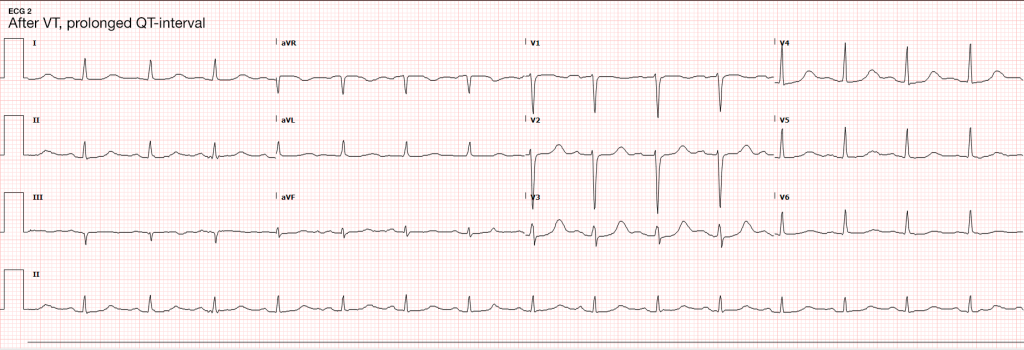
ECG
Imaging
- CXR: Negative acute.
- CT Head: Negative acute.
- CT Cardiac: NICM, EF 35%.
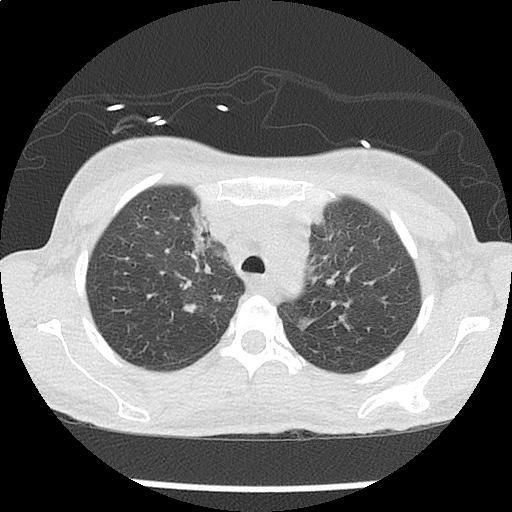
CT Chest non-contrast
- Diffuse patchy GGO (pulmonary edema, atypical pneumonia, alveolar hemorrhage, others).
- Multiple bilateral pulmonary nodules.
- Possible pulmonary arterial hypertension.
Hospital Course
The patient’s evaluation in the emergency department was concerning for severe sepsis secondary to suspected pulmonary source (given association of fever with cough, hypoxia and abnormal chest imaging findings). The patient had persistent alteration in mental status concerning for CNS infection. While preparing for lumbar puncture, cardiac monitoring revealed sustained polymorphic ventricular tachycardia without appreciable pulse. CPR was initiated, amiodarone 150mg IV push administered and at first pulse check a perfusing sinus rhythm was noted with immediate recovery of prior baseline mental status. Amiodarone load was continued and additional potassium sulfate (PO and IV) was administered. Review of telemetry monitoring revealed preceding 30-45 minutes of non-sustained ventricular tachycardia. The patient had two more episodes of sustained ventricular tachycardia requiring defibrillation. The patient was admitted to the medical intensive care unit for continued management.
#Sustained Ventricular Tachycardia
Initially attributed to critical hypokalemia and hypomagnesemia. However, after appropriate repletion serial ECG’s continued to demonstrate prolonged QT interval (possibly acquired secondary to medications, later review revealed multiple promotility agents for treatment of gastroparesis which could contribute to QT-prolongation including erythromycin and metoclopramide, also associated with endocrinopathies). Early echocardiography demonstrated global hypokinesis with estimated EF 30-35%. This was initially attributed to severe sepsis, as well as recurrent defibrillation. However, cardiac CT after resolution of acute illness showed persistent depressed ejection fraction, no evidence of coronary atherosclerosis. The presence of non-ischemic cardiomyopathy (may be attributable to chronic endocrine dysfunction or prior history of methamphetamine abuse) associated with malignant dysrhythmias warranted ICD placement for secondary prevention which the patient was scheduled to receive.
#Severe Sepsis
Attributed to pulmonary source given CT findings, healthcare associated and covered broadly. Mental status gradually improved and returned to baseline. CT head was negative, lumbar puncture deferred.
#Hypokalemia
Unclear etiology. Adrenal insufficiency commonly associated with hyperkalemia and no history of surreptitious fludrocortisone use. Possibly secondary to GI losses. Improved with repletion.
#Autoimmune Polyglandular Syndrome
Started on stress-dose steroids in emergency department. Transiently developed DKA which was reversed appropriately and hydrocortisone was tapered to home regimen. Home levothyroxine was resumed.
Endocrine Emergencies:
Endocrine Emergencies: Hypothyroidism
Symptoms
| Constitutional | Weight gain, cold intolerance, fatigue |
| Cardiopulmonary | Dyspnea, decreased exercise capacity |
| Neuropsychiatric | Impaired concentration and attention |
| Musculoskeletal | Extremity swelling |
| Gastrointestinal | Constipation |
| Reproductive | Irregular menses, erectile dysfunction, decreased libido |
| Integumentary | Coarse hair, dry skin, alopecia, thin nails |
Signs
| Vital signs | Bradycardia, hypothermia |
| Cardiovascular | Prolonged QT, increased ventricular arrhythmia, accelerated CAD, diastolic heart failure, peripheral edema |
| Neurologic | Lethargy, slowed speech, agitation, seizures, ataxia/dysmetria, mononeuropathy, delayed relaxation of reflexes |
| Musculoskeletal | Proximal myopathy, pseudohypertrophy, polyarthralgia |
| Gastrointestinal | Ileus |
Myxedema Coma
- Precipitants
- Critical illness: sepsis (especially PNA), CVA, MI, CHF, trauma, burns
- Endocrine: DKA, hypoglycemia
- Drugs: amiodarone, lithium, phenytoin, rifampin, medication non-adherence
- Environmental: cold exposure
- Recognition
- History: hypothyroidism, thyroidectomy scar and acute precipitating illness
- Hypothermia: temp <95.9°F (or normal in presence of infection)
- AMS: lethargy, confusion, coma, agitation, psychosis, seizures
- Hypotension: refractory to volume resuscitation and pressors
- Bradypnea: with hypercapnia and hypoxia
- Hyponatremia
Management
- Airway protection
- Fluid resuscitation
Thyroid hormone replacement
- Young, otherwise healthy patients: T3 10ug IV q4h
- Elderly, cardiac compromise: 300ug IV x1
- Hydrocortisone: 50-100mg IV q6-8h
- Treat precipitating illness
Interpretation of Thyroid Function Tests
| CONDITION | TSH | T4 |
|---|---|---|
| None | Normal | Normal |
| Hyperthyroidism | Low | High |
| Hypothyroidism | High | Low |
| Subclinical hyperthyroidism | Low | Normal |
| Subclinical hypothyroidism | High | Normal |
| Sick euthyroid | Low | Low |
Endocrine Emergencies: Adrenal Insufficiency
Either primary due to adrenal gland failure (often secondary to autoimmune destruction), or secondary most often due to exogenous glucocorticoid administration (usually requiring more than 30mg/day for > 3wks).
Symptoms
| Constitutional | Weakness, fatigue |
| Gastrointestinal | Anorexia, nausea, cramping |
| Neuropsychiatric | Depression, apathy |
| Reproductive | Amenorrhea, decreased libido |
| Musculoskeletal | Myalgia, arthralgia |
Signs
| General | Hyponatremia, orthostatic hypotension, low-grade fever |
| Primary | Hyperpigmentation, hyperkalemia, hyperchloremia, acidosis |
| Secondary | Hypoglycemia |
Management
- Maintenance
- Hydrocortisone 20mg qAM, 10mg qPM
- Fludrocortisone 50-100ug daily
- Minor illness (x2)
- Hydrocortisone 40mg qAM, 20mg qPM
- Fludrocortisone 50-200ug daily
- Adrenal Crisis
- Dexamethasone 4mg IV or hydrocortisone 100mg IV
- 2-3L 0.9% NaCl
- Treat precipitating illness
Life-Threatening Electrolyte Abnormalities
Critical Hypokalemia
- Causes
- GI losses (diarrhea, laxative use)
- Renal losses (hyperaldosteronism, diuretics)
- Cellular shifts (alkalosis)
- ECG changes
- U-waves 4
- T-wave flattening
- Ventricular arrhythmias (exacerbated with digoxin use)
- Treatment
- Maximum rate 10-20mEq/h with ECG monitoring
- If malignant ventricular arrhythmias or arrest imminent, consider more rapid administration (10mEq over 5 minutes)
Critical Hypomagnesemia
- Causes
- GI, renal losses
- Thyroid dysfunction
- Treatment
- 1-2g IV over 5-60 minutes or IVP for Torsades
Conclusion
Unfortunately, this patient’s comprehensive clinical picture does not fit neatly into a particular category of endocrinologic pathology. Her underlying autoimmune disorder manifests both primary adrenal and thyroid dysfunction. Components of the patient’s presentation are suggestive of critical hypothyroidism (myxedema coma) including alteration in mental status, QT-prolongation and hyponatremia as well as possible precipitant of pneumonia. However, despite elevated TSH, the patient’s free T4 level was within normal range. Also absent was hypoventilation (the patient was appropriately tachypneic for degree of hypoxia and with resultant respiratory alkalosis) or bradycardia/hypothermia.
Similarly, adrenal insufficiency is typically associated with hyperkalemia, whereas our patient had critical hypokalemia that was determined to be at least a contributory factor to her ventricular dysrhythmia. The etiology of the patient’s hypokalemia remained unexplained.
Hyperglycemic Crises
Blurred vision, numbness
HPI
56 year-old male with a history of DM, questionable HTN presenting with blurred vision, numbness of fingertips/toes for 2wks. Associated symptoms include dry mouth, polydipsia/polyuria. He states that these symptoms coincide with elevated measurements of blood glucose at home (>500). He ran out of his diabetes medication (metformin) 8mo ago but states his BG was typically between 100-200 with diet/exercise until 2wks ago. He reports recent dietary indiscretions on a trip to Las Vegas.
He denies fevers/chills, CP/SOB, cough, abdominal pain, N/V, or dysuria.
PMH:
- DM II
- HTN
PSH:
None
FH:
Several maternal family members with DM.
SHx:
- No tobacco/drug use
- 5-6 alcoholic drinks/wk
Meds:
- Metformin 500mg p.o. b.i.d.
Allergies:
NKDA
Physical Exam
| VS: | T 37.8 HR 60 RR 14 BP 165/90 O2 99% RA |
| Gen: | Well-appearing, no acute distress, obese |
| HEENT: | PERRL, EOMI, optic discs sharp b/l, no abnormalities visualized |
| CV: | RRR, normal S1/S2, no M/R/G, no additional heart sounds |
| Lungs: | CTAB, no wheezes/crackles |
| Abd: | +BS, soft, NT/ND, no rebound/guarding |
| Ext: | Warm, well-perfused, 2+ pulses, no clubbing/cyanosis/edema |
| Neuro: | AAOx3, CN II-XII intact |
Labs/Studies
- BMP: 135/3.8/102/24/18/1.1/378
- CBC: 7.4/14.1/42.0/403
- UA: + glucose, – ketones
Assessment/Plan
56M, hx DM with poor medication adherence presenting with vision changes and stocking/glove paresthesias for 2wks after reported dietary indiscretion found to be hyperglycemic. DKA/HHS unlikely given stable vital signs, normal metabolic panel with exception of isolated hyperglycemia (slight hyponatremia likely related to osmotic effect of elevated serum glucose). Also, no evidence of concerning precipitates for hyperglycemic crisis (no CP/SOB, no F/C, no cough, no abdominal pain, no change in mental status). Patient was discharged home with education on importance of medication adherence, refill of metformin, and follow-up with primary care physician for further management of DM and possible hypertension.
Evaluation of hyperglycemic crises in patients with diabetes
Key signs/symptoms of HHS/DKA
- Both: Polyuria, polydipsia, weight loss, hypovolemia (dry MM, skin turgor, tachycardia, hypotension)
- DKA: Short course (<24h), N/V, diffuse abdominal pain, Kussmaul respirations
- HHS: Longer course (days/weeks), altered mental status (lethargy, coma, seizure)
Admission Laboratory Data of Patients with HHS vs. DKA
| DKA | HHS | |
|---|---|---|
| Glucose (mg/dl) | 616 | 930 |
| pH | 7.12 | 7.30 |
| 3-β-hydroxybutyrate (mmol/l) | 9.1 | 1.0 |
| Serum osmolality | 323 | 380 |
| Delta gap (AG-12) | 17 | 11 |
| Na (mEq/l) | 134 | 149 |
| K (mEq/l) | 4.5 | 3.9 |
| Bicarbonate (mEq/l) | 9 | 18 |
Delirium
A 70 year-old female with a PMH of HTN, DM, hyperlipidemia and stage I breast cancer s/p lumpectomy with sentinel LN biopsy several years ago presented for elective surgery complicated by post-operative bleeding. She is now 4 days post-op and was found to be confused, somnolent and occasionally agitated.
HPI
The patient could not be interviewed.
PE
- VS: Stable and within normal limits
- General: unremarkable except for crackles in bilateral lung bases
- MSE: only arouses to sternal rub and becomes agitated, moving all four extremities spontaneously and symmetrically.
- Reflexes: corneal and gag reflexes present, suppresses eye movements with head turn, deep tendon reflexes 3+ throughout UE/LE bilaterally.
Assessment
70 year-old woman with a history of HTN, DM, hyperlipidemia and breast cancer presents with worsening confusion, somnolence and occasional agitation four days after surgery. The combination of significantly altered consciousness and absence of focal neurological findings, all in the setting of a complicated surgical course suggest delirium.
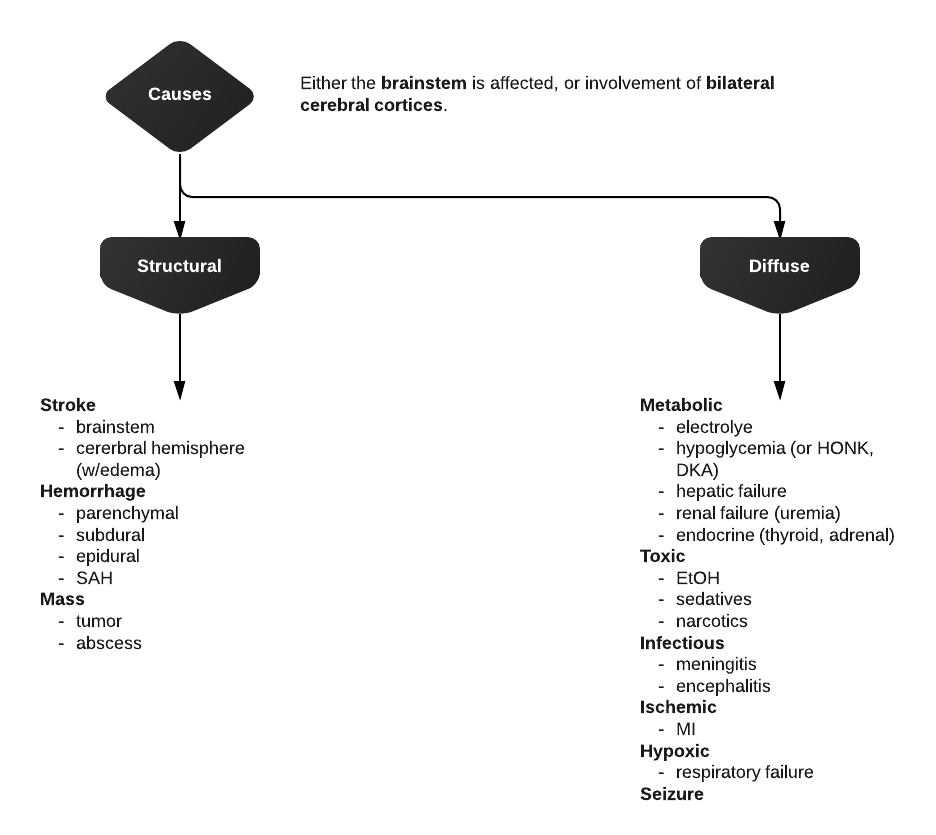
Differential Diagnosis of Altered Mental Status
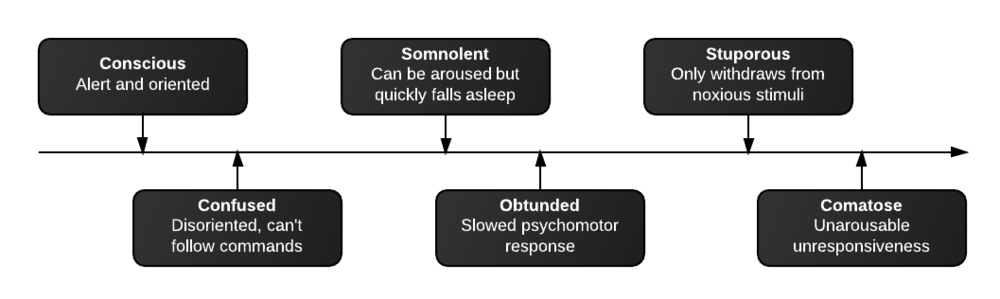
Levels of consciousness
There are different levels of consciousness, they are named in the diagram below but are better described by the characteristics observed.
Initial assessment
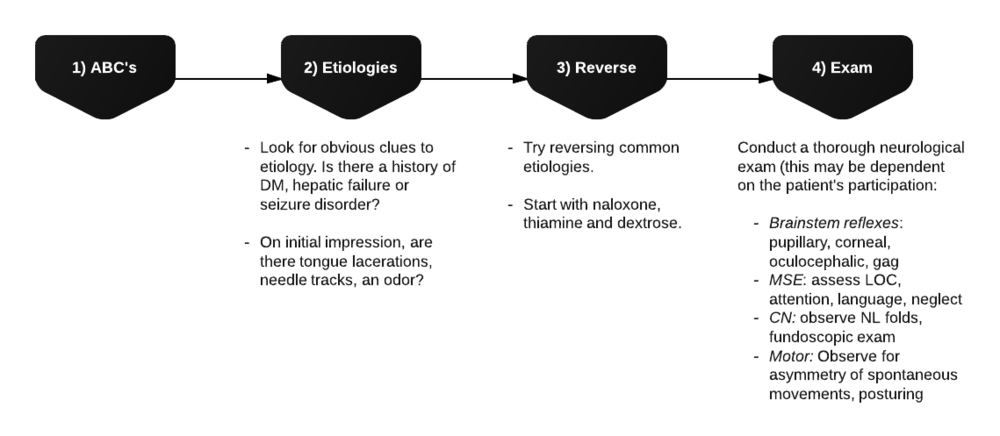
Differential Diagnosis for Altered Mental Status
References
- “The Management of Diabetic Ketoacidosis in
- “Narrative review: ketosis-prone type 2 diabetes mellitus”(PDF). Annals of Internal Medicine. 144 (5): 350–7. doi:10.7326/0003-4819-144-5-200603070-00011. PMID 16520476. Archived (PDF) from the original on 2008-12-05.
- “SGLT2 Inhibitors May Predispose to Ketoacidosis”. The Journal of Clinical Endocrinology & Metabolism. 100 (8): 2849–2852. doi:10.1210/jc.2015-1884. PMC 4525004 . PMID 26086329.
- Diabetic ketoacidosis in adults” (PDF). BMJ (Clinical research ed.). 351: h5660. doi:10.1136/bmj.h5660. PMID 26510442.
- . “Rare complications of pediatric diabetic ketoacidosis”. World journal of diabetes. 6 (1): 167–74. doi:10.4239/wjd.v6.i1.167. PMC 4317308 . PMID 25685287.
- “Hyperglycemic crises in adult patients with diabetes”. Diabetes Care. 32 (7): 1335–43. doi:10.2337/dc09-9032. PMC 2699725 . PMID 19564476. Archived from the original on 2016-06-25.
- Ferri, Fred F. (2010). Ferri’s Differential Diagnosis: A Practical Guide to the Differential Diagnosis of Symptoms, Signs, and Clinical Disorders. Elsevier Health Sciences. p. 146. ISBN 0323076998. Archived from the
- “Calcium block of Na+ channels and its effect on closing rate”. Proceedings of the National Academy of Sciences of the United States of America. 96 (7): 4154–4157. Bibcode:1999PNAS…96.4154A. doi:10.1073/pnas.96.7.4154. PMC 22436 . PMID 10097179.
- Kitabchi AE, Umpierrez GE, Murphy MB, Kreisberg RA (December 2006). “Hyperglycemic crises in adult patients with diabetes: a consensus statement from the American Diabetes Association”. Diabetes Care. 29 (12): 2739–48. doi:10.2337/dc06-9916. PMID 17130218. Archived from the original on 2010-03-27.
- “European Society for Paediatric Endocrinology/Lawson Wilkins Pediatric Endocrine Society consensus statement on diabetic ketoacidosis in children and adolescents”.