How Do I Treat Dry Gangrene/Dry gangrene is a form of coagulative necrosis that develops in ischemic tissue, where the blood supply is inadequate to keep tissue viable. It is not a disease itself, but a symptom of other diseases.[10] Dry gangrene is often due to peripheral artery disease but can be due to acute limb ischemia. As a result, people with arteriosclerosis, high cholesterol, diabetes, and smoking commonly have dry gangrene.
Gangrene localized death of animal soft tissue, caused by prolonged interruption of the blood supply that may result from injury or infection. Diseases in which gangrene is prone to occur include arteriosclerosis, diabetes, Raynaud’s disease, thromboangiitis obliterans (Buerger’s disease), and typhus. It also may occur after severe burns, freezing, or prolonged bed rest (bed sores).
Gangrene is a rapidly progressive life-threatening infection of skeletal muscle caused by clostridia (principally Clostridium perfringens). It is due to wound contamination in the setting of severe tissue trauma, inadequate surgical débridement, immunosuppression, and impaired blood supply. Rarely, nontraumatic gas gangrene caused by Clostridium septicum may occur in patients with occult gastrointestinal malignancies and lead to transient bacteremia.
Gangrene is a type of tissue death caused by a lack of blood supply.[rx] Symptoms may include a change in skin color to red or black, numbness, swelling, pain, skin breakdown, and coolness.[rx] The feet and hands are most commonly affected.[rx] Certain types may present with a fever or sepsis.[rx]
Types of Gangrene

Dry gangrene
- Dry gangrene is a form of coagulative necrosis that develops in ischemic tissue, where the blood supply is inadequate to keep tissue viable. It is not a disease itself, but a symptom of other diseases.[10] Dry gangrene is often due to peripheral artery disease but can be due to acute limb ischemia. As a result, people with arteriosclerosis, high cholesterol, diabetes, and smoking commonly have dry gangrene.[11]
- The affected area becomes cold and numb.
- Initially, the affected area becomes red.
- Then, it develops a brown discoloration.
- Finally, it becomes black and shriveled.
Wet gangrene
- Wet or infected, gangrene is characterized by thriving bacteria and has a poor prognosis (compared to dry gangrene) due to sepsis resulting from the free communication between infected fluid and circulatory fluid. In wet gangrene, the tissue is infected by saprogenic microorganisms (Clostridium perfringens or Bacillus fusiformis, for example), which cause the tissue to swell and emit a bad smell. Wet gangrene usually develops rapidly due to blockage of venous (mainly) or arterial blood flow.[rx] The affected part is saturated with stagnant blood, which promotes the rapid growth of bacteria.
- The affected area becomes swollen and decays.
- It is extremely painful.
- Local oozing occurs.
- It produces a foul-smelling odor.
- It becomes black.
- The affected person develops a fever.
Gas gangrene
- Gas gangrene is a bacterial infection that produces gas within tissues. It can be caused by Clostridium, most commonly alpha toxin-producing C. perfringens, or various nonclostridial species.[rx][rx] The infection spreads rapidly as the gases produced by the bacteria expand and infiltrate healthy tissue in the vicinity. Because of its ability to quickly spread to surrounding tissues, gas gangrene should be treated as a medical emergency.
- A brown-red or bloody discharge may ooze from the affected tissues.
- The gas produced by Clostridia may produce a crackling sensation when the affected area is pressed.
- It becomes swollen, and blisters may develop.
- Pain in the affected area is severe.
- The affected person develops fever, increased heart rate, and rapid breathing if the toxins spread into the bloodstream.
Clinical consideration when gas gangrene is present.
- (A) Localized – crepitant or noncrepitant
- (B) Diffuse – crepitant or noncrepitant together with toxemia
- (A) Bacterial – aerobic androgenic infections; Staphylococcal
fasciitis; anaerobic streptococcal infections - (B) Nonbacterial – mechanical trauma; infiltration from air-hose
injury.
Internal gangrene
- Gangrene that affects one or more of your organs, such as your intestines, gallbladder or appendix, is called internal gangrene. This type of gangrene occurs when blood flow to an internal organ is blocked — for example, when your intestines bulge through a weakened area of muscle in your abdomen (hernia) and become twisted. Internal gangrene may cause fever and severe pain. Left untreated, internal gangrene can be fatal.
Fournier’s gangrene
- Fournier’s gangrene involves genital organs. Men are more often affected, but women can develop this type of gangrene as well. Fournier’s gangrene usually arises due to an infection in the genital area or urinary tract and causes genital pain, tenderness, redness, and swelling.
Progressive bacterial synergistic gangrene (Meleney’s gangrene)
- This rare type of gangrene typically occurs after an operation, with painful skin lesions developing one to two weeks after surgery.
Other Types
- Necrotizing fasciitis, also known as hemolytic streptococcal gangrene, is an infection that spreads deep into the body along tissue planes. It is characterized by infection with S.pyogenes, a gram-positive cocci bacteria.[rx]
- Noma is a gangrene of the face.
- Fournier gangrene is a type of necrotizing fasciitis that usually affects the genitals and groin.[rx]
- Venous limb gangrene may be caused by heparin-induced thrombocytopenia and thrombosis.[rx]
- Severe mesenteric ischemia may result in gangrene of the small intestine.
- Severe ischemic colitis may result in gangrene of the large intestine.

Causes of Gangrene
All forms of gangrene happen because of a loss of blood supply to a certain area. This deprives tissue of oxygen and nutrients, causing the tissue to die.
Dry forms can also result from:
- Vascular problems – Most commonly due to the poor health of arteries and veins in the legs and toes. This usually develops over time due to conditions such as diabetes, peripheral arterial disease, and high blood pressure.
- Severe burns, scalds, and cold – Heat, chemical agents, and extreme cold, including frostbite, can all lead to dry gangrene. Wet gangrene may develop later.
- Raynaud’s disease – There is impaired circulation to the ends of fingers and toes, especially in cold weather. Raynaud’s is implicated in some cases of gangrene.
- Diabetes – Imbalanced blood sugar levels can damage blood vessels and nerves, reducing the oxygen supply to extremities.
- Injury – Deep, crushing, or penetrating wounds that are sustained in conditions that allow bacterial infection can lead to gangrene. Examples are war zones and railway, machinery, and street accidents if lacerated and bruised tissues are contaminated.
- Dry gangrene – If the area is infected with bacteria.
- Embolism – The sudden blockage of an artery can lead to dry gangrene, but it also increases the risk of infection, and therefore wet gangrene.
- Immune deficiency – If an immune system is weakened, for example by HIV, diabetes, long-time alcohol or drug abuse, or recent chemotherapy or radiotherapy, minor infections escalate more quickly and can become gangrenous.
Anorectal Causes
- Trauma
- Ischiorectal, perirectal, or perianal abscesses, appendicitis,
- diverticulitis, colonic perforations
- Perianal fistulotomy, perianal biopsy, rectal biopsy, hemorrhoidectomy, anal fissures excision
- Steroid enemas for radiation proctitis
- Rectal cancer
Genitourinary Causes
- Trauma
- Urethral strictures with urinary extravasation
- Urethral catheterization or instrumentation, penile implants insertion, prostatic biopsy, vasectomy, hydrocele aspiration, genital piercing, intracavernosal cocaine injection
- Periurethral infection; chronic urinary tract infections
- Epididymitis or orchitis
- Penile artificial implant, foreign body
- Hemipelvectomy
- Cancer invasion to the external genitalia
- Diabetes,
- Peripheral arterial disease,
- Smoking, major trauma,
- Alcoholism, HIV/AIDS, frostbite, and Raynaud’s syndrome.[rx][rx]
Symptoms of Gangrene
- Coldness and numbness in the affected area
- Pain in or beyond the affected area
- Redness and swelling around a wound (this is often present when wet gangrene develops)
- Sores that keep cropping up in the same place
- Initial redness and swelling
- Either a loss of sensation or severe pain in the affected area
- Sores or blisters that bleed or release a dirty-looking or foul-smelling discharge (if the gangrene is caused by an infection)
- The skin becomes cold and pale
- Persistent, unexplained fever, with a temperature higher than 100.4°F (38°C)
- A bad-smelling wound
- Striking discoloration of the skin, with shades of greenish-black, blue, red, or bronze
- Pus or discharge from a wound
- Blisters and a crackling feeling under the skin
- Confusion, pain, fever, and low blood pressure, especially if the gangrene is internal
- Shock
[stextbox id=’custom’]
Differences in features of dry gangrene, wet gangrene, and gas gangrene
| Feature | Dry gangrene | Wet gangrene | Gas gangrene |
|---|---|---|---|
| Site | Commonly limbs | More common in bowel | Limbs |
| Mechanism | Arterial occlusion | More commonly venous obstruction | Gases produced by Clostridium bacteria |
| Macroscopy | Organ dry, shrunken, and black | Part moist, soft, swollen, rotten, and dark | Organ red, cold, pale, numb, shriveled up, and auto-amputation |
| Putrefaction | Limited due to very little blood supply | Marked due to congestion of organ with blood | Marked due to bacteria and infiltration of gases produced by them in tissues |
| Line of demarcation | Present at the junction between healthy and gangrenous parts | No clear-cut line of demarcation | No clear-cut line of demarcation |
| Bacteria | Bacteria fail to survive | Numerous present | Major cause |
| Prognosis | Generally better due to little septicemia | Generally poor due to profound toxemia | Generally poor due to quickly spread to the surrounding tissues |
Note: Data from NHP.gov.in.11
[/stextbox]
Diagnosis of Gangrene
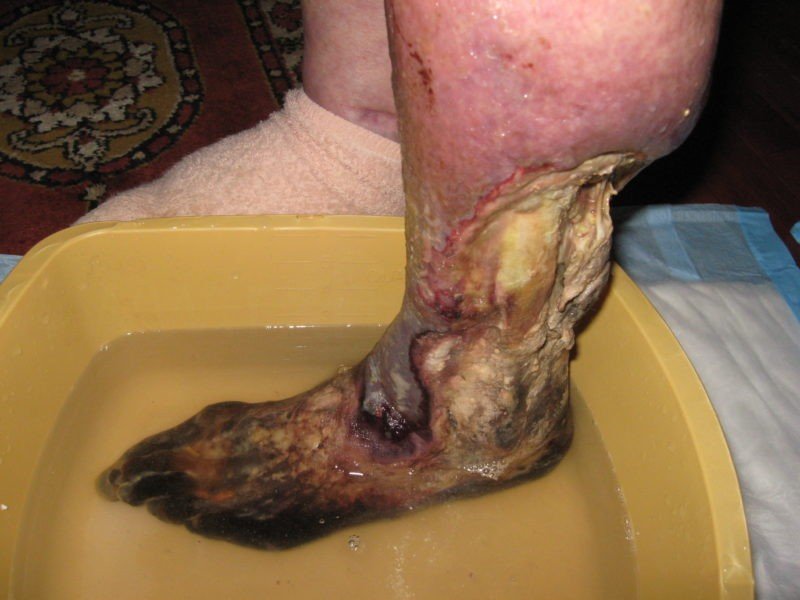
Laboratory Studies
The following studies are indicated in patients Fournier gangrene.
- CBC with the differential count.
- Electrolytes, BUN, creatinine, blood glucose levels: acidosis with hyperglycemia or hypoglycemia may be present. Dehydration occurs as the disease progresses.
- ABG sampling to provide a more accurate assessment of acid/base disturbance.
- Blood and urine cultures.
- Disseminated intravascular coagulation (DIC) panel (coagulation studies, fibrinogen/fibrin degradation product levels) to find evidence of severe sepsis.
- Cultures of any open wound or abscess.
- Fluid or tissue culture – where a small tissue or fluid sample from the affected area is tested to find out which bacteria are responsible for the condition and determine the most effective antibiotic to treat it with
- Blood cultures – where a sample of blood is taken and put into special culture bottles and placed in a warm environment (incubated) to encourage the growth of bacteria so they can be examined further
- Imaging tests – a range of imaging tests, such as X-rays, magnetic resonance imaging (MRI) scans or computerized tomography (CT) scans can be used to confirm the presence and spread of gangrene; these tests can also be used to study blood vessels so any blockages can be identified
- Ankle-brachial index test – This test helps in determining arterial blood circulation and blood pressure in the lower extremities.[rx]
- Carotid duplex test – This test is done to know the rate of blood flow through carotid arteries. It helps in exploring the presence of any plaques that may cause carotid artery disease.[rx]
- Computed angiography and magnetic resonance angiography – These are the computerized imaging tests that are useful in studying in the blood vessels. These techniques help the vascular surgeons to know the severity of the disease.[rx]
- Duplex ultrasound – Duplex ultrasound is used to assess the blood flow status in blood vessels. With this technique, vascular surgeons easily explore the existence of an occlusion or clot and plan the treatment.[rx]
- Skin perfusion pressure (SPP) and skin vascular resistance – SPP and skin vascular resistance measurements also help in distinguishing the patients who require vascular reconstruction or major amputation and the patients who only require foot care or require minor amputation [rx]. A prospective, double-blinded study by Castronuovo et al concluded that in ~80% cases, SPP helps in diagnosing the critical limb ischemia accurately.[rx],[rx]
- Ultrasonography – A US finding in Fournier gangrene is a thickened wall containing hyperechoic foci that demonstrate reverberation artifacts, causing “dirty” shadowing that represents gas within the scrotal wall. Evidence of gas within the scrotal wall may be seen prior to clinical crepitus. Reactive unilateral or bilateral hydroceles may also be present. If testicular involvement occurs, there is likely an intraabdominal or retroperitoneal source of infection. US is also useful in differentiating Fournier gangrene from an inguinoscrotal incarcerated hernia; in the latter condition, gas is observed in the obstructed bowel lumen, away from the scrotal wall [rx].
- Computed Tomography – The CT features of Fournier gangrene include soft-tissue thickening and inflammation. CT can demonstrate asymmetric fascial thickening, any coexisting fluid collection or abscess, fat stranding around the involved structures, and subcutaneous emphysema secondary to gas-forming bacteria. The underlying cause of the Fournier gangrene, such as a perianal abscess, a fistulous tract, or an intraabdominal or retroperitoneal infectious process, may also be demonstrated at CT. In early Fournier gangrene, CT can depict progressive soft-tissue infiltration, possibly with no evidence of subcutaneous emphysema. Because the infection progresses rapidly, the early stage with lack of subcutaneous emphysema is brief and is rarely seen at CT [rx].
Treatment of Gangrene
Broad-Spectrum Antibiotics Coverage
- Empiric broad-spectrum antibiotic therapy should be instituted as soon as possible until the culture results could make adjusted the therapy. The antibiotic regimen chosen must have a high degree of effectiveness against staphylococcal and streptococcal bacteria, gram-negative, coliforms, pseudomonas, Bacteroides, and clostridium.
- Classically Triple therapy is usually recommended. Third generation cefalosporins or aminoglycosides, plus penicillin and metronidazole.
- Clindamycin may be used as it is shown to suppress toxin production and modulate cytokine production; also use of linezolid, daptomycin, and tigecycline is warranted in cases of previous hospitalizations with prolonged antibiotic therapy which may lead to resistant Bacteroides [rx].
[stextbox id=’custom’]
Pharmacologic approaches for gangrene management
| Pharmacologic approach | Drugs class examples | Mechanism of action |
|---|---|---|
| Pain management | Opioids and opioid-like analgesics Morphine, oxycodone, dextromethorphan, tapentadol, tramadol | Mimic the actions of endogenous opioid peptides by interacting with mu, delta, or kappa opioid receptors |
| Topical medications: capsaicin, lidocaine | Provide local action on the skin to relieve pain | |
| Circulation management | Antiplatelet agents: aspirin, clopidogrel, prasugrel, ticlopidine, dipyridamole, abciximab, eptifibatide, tirofiban, ticagrelor, vorapaxar | Prevent the aggregation of platelets and fibrinogenesis |
| Anticoagulants: heparin, fondaparinux, danaparoid, bishydroxycoumarin, warfarin, acenocoumarol, phenindione | Cause activation of anticlotting factors, direct inhibition of thrombin, inhibition of synthesis of blood coagulation factor precursors (zymogens), and activation of protein C | |
| Fibrinolytic agents: streptokinase, urokinase, alteplase, reteplase, tenecteplase | Cause lysis of thrombi/clot to recanalize the occluded vessels | |
| Antibiotics | Penicillins: flucloxacillin | Inhibit bacterial cell wall synthesis by binding to specific penicillin-binding proteins located inside the bacterial cell wall |
| Fluoroquinolones: ciprofloxacin | Inhibit topoisomerase II (DNA gyrase) and topoisomerase IV, which are required for bacterial DNA replication, transcription, repair, strand supercoiling repair, and recombination | |
| Antiprotozoals: metronidazole | In reduced form, they covalently bind to DNA, disrupt its helix structure, inhibiting bacterial nucleic acid synthesis, and cause bacterial cell death | |
| Carbapenems: ertapenem, meropenem | Show bactericidal activity by inhibiting the bacterial cell wall synthesis | |
| Glycopeptides: teicoplanin, vancomycin | Inhibit the bacterial cell wall synthesis and cause cell death | |
| Tetracyclines: doxycycline | Reversibly bind to 30S ribosomal subunits and possibly to 50S subunits, block the binding of aminoacyl tRNA to mRNA, and inhibit bacterial protein synthesis | |
| Lincosamides: clindamycin | Inhibit bacterial protein synthesis by binding to 50S ribosomal subunits of the bacteria | |
| Oxazolidinones: linezolid | Selectively inhibit bacterial protein synthesis by binding to bacterial ribosomes and prevent the formation of a functional 70S initiation complex |
[/stextbox]
Early IV antibiotics
- Early IV antibiotics with early surgical debridement followed by hyperbaric oxygen therapy can salvage patients with an otherwise nearly always fatal disease. Intravenous antibiotics and early surgical debridement of the necrotic tissue reduce fatality rate to about 30%. With the addition of hyperbaric oxygen therapy, this can be reduced down to 5 to 10%.
- Hyperbaric oxygen therapy helps by halting exotoxin production by the bacteria, helps to improve the bactericidal effect of the antibiotic, treats the tissue ischemia, improves reperfusion injury of the tissue, and promotes the activation and migration of stem cells and polymorphonuclear cells.
Pain management
- Gangrene is usually associated with intermittent claudication in the limbs of patients. Thus, it is important to effectively manage the pain to let the patient continue exercises to improve circulation.
- Opioid analgesics are recommended for pain associated with chronic limb ischemia. Apart from vascular factors, neuropathic pain should also be managed as a priority.[rx]
Circulation management
As the senile/dry gangrene is a consequence of ischemia, improving the blood circulation in limbs helps overcome peripheral artery disease.[rx] As per the American Diabetes Association, antiplatelet therapy or platelet aggregation inhibitors are highly recommended for preventing the vascular complications in diabetes patients.[rx] In some cases, surgery may be carried out to restore the blood flow to the affected area. The main techniques used to achieve this are:
- Bypass surgery – where the surgeon redirects the flow of blood and bypasses the blockage by connecting (grafting) one of your veins to a healthy part of an artery
- Angioplasty – where a tiny balloon is placed into a narrow or blocked artery and is inflated to open up the vessel; a small metal tube, known as a stent, may also be inserted into the artery to help keep it open
Research suggests that both techniques are equally effective in restoring blood flow and preventing the need for amputation in the short-term. An angioplasty has the advantage of having a faster recovery time than bypass surgery, although it may not be as effective in the long-term as bypass surgery.
Lipid-lowering agents
- Dyslipidemia plays a major role in the progression of diabetic toe gangrene. Thus, diabetes patients should undergo a regular lipid profile check-up. In a descriptive case series study performed by Memon et al, 55.11% cases were reported to have abnormal lipid profile and 44.89% cases had lipid profile within the normal range.
- As per Wagner’s scale, the percentage of patients with superficial ulcers (Grade I), ulcer extension (Grade II), deep ulcer with abscess (Grade III), gangrene of ore foot (Grade IV), and extensive gangrene foot (Grade V) was found to be 30.61%, 19.39%, 21.42%, 16.33%, and 12.25% respectively. A significant difference (p=0.001) was found in the gangrenous diabetic foot, grade IV and grade V.[rx]
Larval debridement therapy (biosurgery)
- In some cases, it may be possible to use larval debridement therapy, also known as biosurgery, instead of conventional surgery to remove the dead tissue. Certain types of fly larvae are ideal for this because they feed on dead and infected tissue but leave healthy tissue alone. They also help fight infection by releasing substances that kill bacteria and stimulate the healing process.
- Maggots used for larval therapy are specially bred in a laboratory using eggs that have been treated to remove bacteria. The maggots are placed on the wound and covered with gauze, under a firm dressing, which keeps them on the wound (and out of sight). After a few days, the dressing is cut away and the maggots are removed. Medical studies have shown larval debridement therapy can achieve more effective results than surgical debridement. However, because of the nature of this type of treatment, many people are reluctant to try it.
Exercise
- Apart from drugs, in dry gangrene patients with peripheral arterial disease, guideline-directed management and therapy should be followed to decrease arterial occlusion or impaired perfusion, prevent the progression of chronic critical limb ischemia, and improve the functional status of affected limbs.
- This involves exercises which are done under structured or unstructured programs. Structured exercise programs include intermittent walking followed by alternate rest time. These are organized in the health care facilities and are supervised by a trained health care professional. Unstructured home-based exercise programs also include walking as a major exercise without any supervisor’s guidance.[rx,rx]
Massage therapy
- Massage Therapy is also recommended to improve the circulation in limbs. Only light pressure massage is given to the affected limb to avoid any clot formation. Massage should be cautiously done in patients with a stent, with special instructions given by the health care professional.[rx]
Fasciotomy
- It may be necessary to relieve compartment pressures. As the infection progresses into deep tissue along and under the fascia tissue compartment pressures increase, which perpetuates further tissue ischemia and necrosis. Surgical debridement should focus on removing all the necrotic tissue, and foreign bodies such as soil, debris, and shrapnel. It is also important to irrigate the wounds with copious amounts of sterile normal saline.
Hyperbaric oxygen therapy
- It should be added to standard therapy of antibiotics and surgical debridement to help improve survival.[rx][rx] It is important to have coordinated care of these critically ill patients with an intensivist, general surgeon, orthopedic surgeon, urologist (in the setting of Fournier’s gangrene of the testicles and perineal structures), gynecologist (in the setting of uterine gas gangrene), infectious disease specialist, hematologist/oncologist, gastroenterologist (in the setting of spontaneous gas gangrene), and hyperbaric oxygen therapy specialist. The flow of consultation starts with usually an emergency department provider and early recognition of the disease.
Conventional Radiography
- At radiography, hyperlucencies representing soft tissue gas may be seen in the region overlying the scrotum or perineum. Subcutaneous emphysema may be seen extending from the scrotum and perineum to the inguinal regions, anterior abdominal wall, and thighs.
- However, the absence of subcutaneous air in the scrotum or perineum does not exclude the diagnosis of Fournier gangrene. Up to 90% of patients with Fournier gangrene have been reported to have subcutaneous emphysema so that at least 10% do not demonstrate this finding [rx].
- Radiography may also demonstrate significant swelling of scrotal soft tissue. Deep fascial gas is rarely seen at radiography, which represents a significant weakness of this modality in the diagnosis and evaluation of Fournier gangrene [rx].
Radical Surgical Debridement
- A debridement of the necrotic tissue as soon as possible it is widely recommended Laor et al. found no significant difference between the onset time of symptoms, early surgical treatment, and mortality, but other studies from Kabay et al. [rx] and Korkut et al. [rx] show that this time interval should be as short as possible.
- Debridement of deep fascia and muscle is not usually required as these areas are rarely involved similar to testes. Debridement should be stopped when the separation of the skin and the subcutaneous is not performed easily because the cutaneous necrosis is not a good marker. Multiple surgical debridements is the rule rather than the exception, with an average of 3.5 procedures required per patient [rx]
Fecal and Urinary Diversion
- Colostomy has been used for fecal diversion in cases of severe perineal involvement. The rationale for rectal diversion includes a decrease in the number of germs in the perineal region and improved wound healing. Justifications for its construction are anal sphincter involving, fecal incontinence, or continues fecal contamination of the wound’s margins. In several papers, the percentage of patients with a colostomy is around 15% depending on the series [rx].
Topical Therapy
- There have been reports of the use of honey to aid wound healing. Honey has a low pH of 3.6 and contains enzymes which digest necrotic tissues it also has antibacterial property due to phenolic acid. These changes occur within a week of applying honey to the wound. Unfortunately, there is no randomized study on the efficacy of honey in these special situations. [rx]
Hyperbaric Oxygen Therapy
- Hyperbaric oxygen therapy implies placing the patient in an environment of increased ambient pressure while breathing 100% oxygen, resulting in enhanced oxygenation of the arterial blood and tissues and demonstrated benefits of hyperbaric oxygen include adequate oxygenation for optimal neutrophil phagocytic function, inhibition of anaerobic growth, increased fibroblast proliferation and angiogenesis, reduction of edema by vasoconstriction, and increased intracellular antibiotics transportation [rx].
Vacuum-Assisted Closure
- With the recent advent of the vacuum-assisted closure (VAC) system dressing, there seems to be a dramatic improvement with minimizing skin defects and speeding tissue healing. It simply works by exposing a wound to subatmospheric pressure for an extended period to promote debridement and healing.
- Weinfeld et al. treated four consecutive cases using negative pressure dressings (VAC) to bolster skin grafts in male genital reconstruction.
Plastic Reconstruction
- Various workers have used different techniques to provide skin cover including transplantation of testes, free skin grafts, axial groin flaps, and myocutaneous flaps. Split thickness skin graft seems to be the treatment of choice in treating perineal and scrotal skin defects.
Home Exercise
- A healthy, well-balanced diet and regular exercise will keep your blood pressure and cholesterol levels at a healthy level, helping prevent your blood vessels become damaged.
- Unless advised otherwise by your doctor, you should be aiming for at least 150 minutes (2.5 hours) of moderately intense physical exercise a week.
Moderate-intensity physical activity is any activity that increases your heart and breathing rate. It may make you sweat but you’ll still be able to hold a normal conversation. Examples include:
- fast walking
- cycling on level ground or with few hills
- swimming
- tennis
You should choose physical activities you enjoy because you’re more likely to continue doing them. It’s probably unrealistic to meet these exercise targets immediately if you haven’t exercised much in the past. Aim to start gradually and build up the amount of exercise you do overtime.
Diet
- Eating an unhealthy diet high in fat will make any existing atherosclerosis worse and increase your risk of developing gangrene.
- Continuing to eat high-fat foods will cause more fatty plaques to build-up in your arteries. This is because fatty foods contain cholesterol.
There are 2 types of fat-saturated and unsaturated. Avoid foods that contain saturated fats because they increase levels of “bad cholesterol” in your blood.
Foods high in saturated fat include:
- meat pies
- sausages and fatty cuts of meat
- butter
- ghee (a type of butter often used in Indian cooking)
- lard
- cream
- hard cheese
- cakes and biscuits
- food containing coconut or palm oil
Prevention of Gangrene
- Our emergency clinicians should be aware of this severe and potentially fatal infectious disease and should not delay treatment or prompt orthopedic surgery consultation. Gas gangrene, while rare in now peace days, can be a devastating complication of almost any small wound or surgical procedure even one as common as closed reduction of fractures. It is our experience that we should give sufficient extension of the wound to provide adequate visualization of the surgical field so as to be certain that all the necrotic or foreign material has been removed.
- Strict aseptic techniques should be observed for even the most minor procedure. Clostridial spores are ubiquitous and can reside in hospital environments, possibly on surgeons’ hands, patients’ skin, topical application, and so on.
- The best way to prevent gas gangrene is meticulous wound debridement and delayed closure for all potentially contaminated wounds regardless of closed or open fractures.
- Once gas gangrene is diagnosed, careful and adequate debridement should be instituted immediately to avoid further deterioration excision of necrotic tissue still the cornerstone of treatment, which should be involved with antibiotics and all other supportive treatments.
- Systematic resuscitative efforts should be instituted immediately in whom the diagnosis of incipient gas gangrene is even considered. This cannot be overemphasized.
- Recognized that gas gangrene may occur spontaneously and often in an immunocompromised patient, postoperative wounds may also develop gas gangrene due to the local soft tissue damage and decreasing blood supply.
- Keep wounds clean and sterile by cleaning all wounds thoroughly with an antiseptic solution.
- Watch for signs of infection, such as pus, redness, swelling, or unusual pain.
- Consult a health-care provider if any wound becomes infected.
- People with diabetes should control their blood sugar levels with proper medication.
- Education about proper foot care is vital for people with diabetes. They should routinely examine their feet for any signs of injury or change in skin color. Any small injury should be immediately cared for. They should keep their nails trimmed and wear comfortable well-fitting shoes.
References
[bg_collapse view=”button-orange” color=”#4a4949″ expand_text=”Show More” collapse_text=”Show Less” ]
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3830836/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4580094/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3518952/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5987754/
- https://www.ncbi.nlm.nih.gov/books/NBK537030/
- https://en.wikipedia.org/wiki/Gangrene
- https://www.ncbi.nlm.nih.gov/pubmed/26445600
- https://www.ncbi.nlm.nih.gov/pubmed/12206606
- https://www.nlm.nih.gov/medlineplus/ency/article/007393.htm
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2743684
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5987754
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5477786
- http://onlinelibrary.wiley.com/resolve/openurl?
- https://www.idf.org/e-library/20-atlas-5th-edition.html
- https://www.sciencedirect.com/topics/neuroscience/gangrene
- http://apps.who.int/iris/bitstream/10665/204871/1/9789241565257_eng.pdf
- https://www.intechopen.com/books/diabetic-foot-and-gangrene
- https://www.nhs.uk/conditions/gangrene/symptoms/
- https://patient.info/doctor/gangrene
- http://www.civilwarmedicalbooks.com/hospital_gangrene_civil_war.html
- https://www.diabetes.co.uk/diabetes-complications/gangrene-and-diabetes.html
- https://www.medicinenet.com/gangrene/article.htm
- https://www.medicalnewstoday.com/articles/158770.php
- https://www.mayoclinic.org/diseases-conditions/gangrene/diagnosis-treatment/drc-20352573
- https://www.healthline.com/health/gangrene
- https://www.emedicinehealth.com/gangrene/article_em.htm
- https://www.hopkinsmedicine.org/health/conditions-and-diseases/gangrene
- https://www.medicinenet.com/gangrene/article.htm
- https://www.britannica.com/science/gangrene
[/bg_collapse]
